TIMESCALE 1 Day
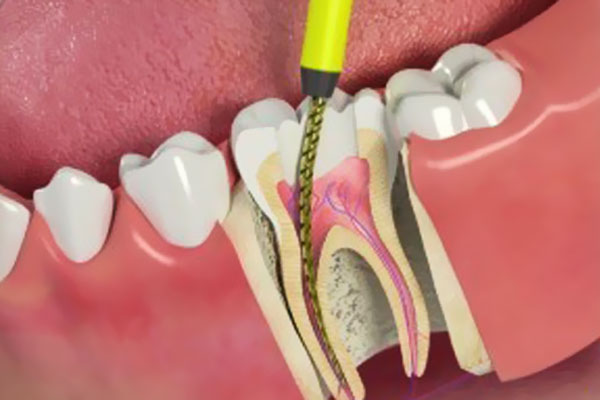
A root canal is a common procedure used to treat inflammation or infection of the tooth’s sensitive inner pulp tissue, which is made up of blood vessels and nerve fibers. Pulp inflammation can result from a number of causes including deep decay, cracked teeth, or trauma. While many feel uneasy about the idea of a root canal, the procedure is a safe and straightforward way to remove diseased pulp tissue and is a better alternative to tooth extraction.
Reasons for root canal treatment
The following are some of the most frequently cited reasons for root canal treatment.
Deep tooth decay
Tooth decay is a bacterial infection of the tooth in which acid eats away at the enamel and dentin of the tooth. If this decay is not treated in its early stages, it will eventually spread until it reaches the pulp of the tooth, resulting in inflammation and infection of the pulp, often pain, and ultimately, death of the tooth. For severe tooth decay that has reached the tooth pulp, your dentist may recommend a root canal. During a root canal procedure, the damaged parts of the tooth and the entirety of the diseased pulp will be removed, medication may be placed to clear any active infection, and the root will be filled and sealed using a rubber-like material. Afterwards the tooth needs to be restored to chewing function with a filling or crown.
Tooth abscess
Sometimes the infection of the pulp will spread beyond the confines of a root canal system and into the bone and soft tissues surrounding the tooth root. This is referred to as an abscess. With an abscess you may notice swelling or a bad taste inside the mouth around the infected tooth. In this scenario, root canal therapy is needed in order to clear the infection in the tooth, bone, and soft tissue and save the tooth. Unfortunately, the only other alternative is tooth extraction.
Fractured or traumatized tooth
When a tooth becomes cracked or fractured to a point where the inner pulp is harmed or exposed to bacteria, a root canal procedure may be necessary.
The need for a root canal will depend on the type of fracture and its severity – a dentist or endodontist will be able to evaluate your tooth and recommend the best treatment option. It’s also important to note that sometimes trauma to the tooth can result in pulp death without there being a fracture in the tooth. In this scenario, symptoms may include pain or abscess, and a root canal will be needed.
Resorption
Dental resorption is a condition in which the inside or outside of the tooth root begins to dissolve. It is most commonly seen in baby tooth roots where they slowly dissolve over time to make room for permanent teeth. Resorption is uncommon in adult teeth and is believed to be caused by tooth trauma, pulp infection, or orthodontic treatment, although sometimes it can occur with no apparent cause. There are two primary types of dental resorption:
- Internal tooth resorption: Where the tooth is dissolving from inside the pulp towards the outside of the tooth.
- External (apical) tooth resorption: Where the tooth’s root begins to dissolve from the outside.
Resorption can often be successfully treated with root canal treatment. There are usually no obvious symptoms – like pain – but the issue can usually be diagnosed with a routine X-ray exam. It is best treated when diagnosed early, so regular dental visits are important.
Multiple restorations of a tooth
Each time a tooth is restored there is going to be some trauma to the tooth and pulp. This is especially true for large, deep fillings. Sometimes this can lead to a condition called chronic pulpitis where the dental pulp is continually inflamed. Over time, the pulp may eventually die, and root canal treatment will be necessary to save the tooth. Additionally, old fillings or crowns may become cracked and leak, allowing bacteria from the mouth to invade the pulp. This scenario will also warrant a root canal.
Endodontic retreatment
Occasionally, a tooth treated with root canal therapy or another type of restorative procedure may fail to heal correctly and become painful or infected over a matter of months, or years, following the original procedure. When this happens, your dentist or endodontist may need to perform a root canal (perhaps for the second time) to save the tooth that didn’t heal properly. This additional procedure is typically very successful and is able to diminish any pain or discomfort, while promoting correct healing.5